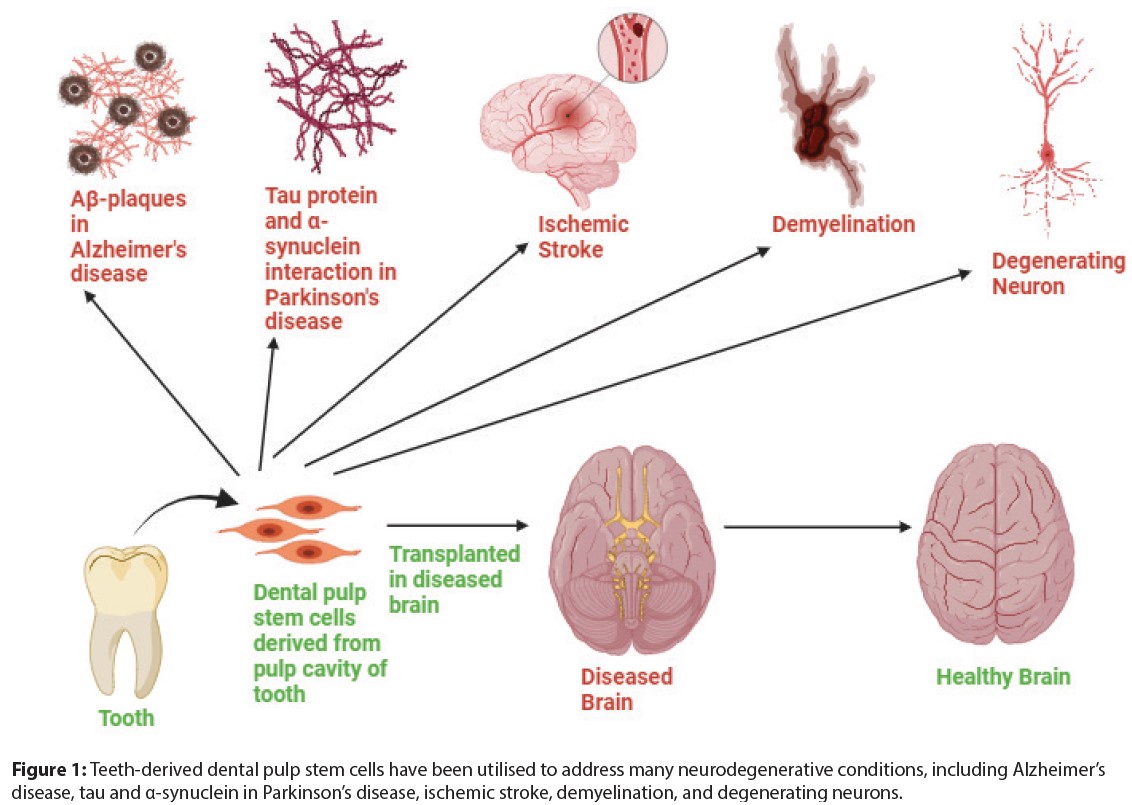
Unlocking the Potential of Dental Pulp Stem Cells: Neuroprotective and Regenerative Insights for Treating Neurological Diseases
Main Article Content
Abstract
Neurological illnesses impose a significant global health burden, with limited treatment options currently available. Recent advances in regenerative medicine have sparked interest in exploring various stem cell sources for neurological disorder treatment. Dental pulp stem cells (DPSCs) have emerged as a promising option due to their neural crest origin, multilineage differentiation capability, and accessibility through routine dental procedures. This review delves into our current understanding of DPSC function concerning neurological diseases, examining their neuroprotective and regenerative potential. It elucidates how DPSCs can differentiate into neural-like cells and release trophic substances that enhance the survival and functionality of neurons. Furthermore, the review explores the mechanisms underlying DPSCs' neuroprotective effects, shedding light on their immunomodulatory characteristics and ability to regulate inflammatory responses in the central nervous system. The challenges and potential avenues for utilizing DPSCs in neurological disorder treatment are also discussed, emphasizing the importance of large-scale clinical trials, ethical considerations, and well-defined procedures.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
The Journals licensing terms of CC-BY-NC-SA 4.0 speaks that you are free to Share (copy and redistribute the material in any medium or format), Adapt (remix, transform, and build upon the material) under proper terms of Attribution (You must give appropriate credit, provide a link to the license, and indicate if changes were made. You may do so in any reasonable manner, but not in any way that suggests the licensor endorses you or your use.), NonCommercial (You may not use the material for commercial purposes.), ShareAlike (If you remix, transform, or build upon the material, you must distribute your contributions under the same license as the original.) and No additional restrictions (You may not apply legal terms or technological measures that legally restrict others from doing anything the license permits.)
References
Al Madhoun A, Sindhu S, Haddad D, Atari M, Ahmad R, Al-Mulla F. Dental Pulp Stem Cells Derived From Adult Human Third Molar Tooth: A Brief Review. Front Cell Dev Biol. 2021;9:717624. Published 2021 Oct 12. doi:10.3389/fcell.2021.717624
Andrukhov O, Behm C, Blufstein A, Rausch-Fan X. Immunomodulatory properties of dental tissue-derived mesenchymal stem cells: Implication in disease and tissue regeneration. World J Stem Cells. 2019;11(9):604-617. doi:10.4252/wjsc.v11.i9.604
Andrukhov O, Behm C, Blufstein A, Rausch-Fan X. Immunomodulatory properties of dental tissue-derived mesenchymal stem cells: Implication in disease and tissue regeneration. World J Stem Cells. 2019;11(9):604-617. doi:10.4252/wjsc.v11.i9.604
Apel C, Forlenza OV, de Paula VJ, et al. The neuroprotective effect of dental pulp cells in models of Alzheimer's and Parkinson's disease. J Neural Transm (Vienna). 2009;116(1):71-78. doi:10.1007/s00702-008-0135-3
Cummings JL, Zhong K, Kinney JW, et al. Double-blind, placebo-controlled, proof-of-concept trial of bexarotene Xin moderate Alzheimer's disease. Alzheimers Res Ther. 2016;8:4. Published 2016 Jan 29. doi:10.1186/s13195-016-0173-2
Fatima N, Khan AA, Vishwakarma SK. Immunophenotypic and Molecular Analysis of Human Dental Pulp Stem Cells Potential for Neurogenic Differentiation. Contemp Clin Dent. 2017;8(1):81-89. doi:10.4103/ccd.ccd_998_16
Fujii H, Matsubara K, Sakai K, et al. Mazzini L, Gelati M, Profico DC, et al. Results from Phase I Clinical Trial with Intraspinal Injection of Neural Stem Cells in Amyotrophic Lateral Sclerosis: A Long-Term Outcome. Stem Cells Transl Med. 2019;8(9):887-897. doi:10.1002/sctm.18-0154 Brain Res. 2015;1613:59-72. doi:10.1016/j.brainres.2015.04.001
Gnanasegaran N, Govindasamy V, Mani V, Abu Kasim NH. Neuroimmunomodulatory properties of DPSCs in an in vitro model of Parkinson's disease. IUBMB Life. 2017;69(9):689-699. doi:10.1002/iub.1655
Gonmanee T, Thonabulsombat C, Vongsavan K, Sritanaudomchai H. Differentiation of stem cells from human deciduous and permanent teeth into spiral ganglion neuron-like cells. Arch Oral Biol. 2018;88:34-41. doi:10.1016/j.archoralbio.2018.01.011
Graziano A, d'Aquino R, Laino G, Papaccio G. Dental pulp stem cells: a promising tool for bone regeneration [published correction appears in Stem Cell Rev. 2008 Spring;4(1):65]. Stem Cell Rev. 2008;4(1):21-26. doi:10.1007/s12015-008-9013-5
Gupta UC. Informed consent in clinical research: Revisiting few concepts and areas. Perspect Clin Res. 2013;4(1):26-32. doi:10.4103/2229-3485.106373
Hoang DM, Pham PT, Bach TQ, et al. Stem cell-based therapy for human diseases. Signal Transduct Target Ther. 2022;7(1):272. Published 2022 Aug 6. doi:10.1038/s41392-022-01134-4
Jin K, Galvan V. Endogenous neural stem cells in the adult brain. J Neuroimmune Pharmacol. 2007;2(3):236-242. doi:10.1007/s11481-007-9076-0
Lamptey RNL, Chaulagain B, Trivedi R, Gothwal A, Layek B, Singh J. A Review of the Common Neurodegenerative Disorders: Current Therapeutic Approaches and the Potential Role of Nanotherapeutics. Int J Mol Sci. 2022;23(3):1851. Published 2022 Feb 6. doi:10.3390/ijms23031851
Lo B, Parham L. Ethical issues in stem cell research. Endocr Rev. 2009;30(3):204-213. doi:10.1210/er.2008-0031
Luo L, He Y, Wang X, et al. Potential Roles of Dental Pulp Stem Cells in Neural Regeneration and Repair. Stem Cells Int. 2018;2018:1731289. Published 2018 May 7. doi:10.1155/2018/1731289
Luo L, He Y, Wang X, et al. Potential Roles of Dental Pulp Stem Cells in Neural Regeneration and Repair. Stem Cells Int. 2018;2018:1731289. Published 2018 May 7. doi:10.1155/2018/1731289
Mahla RS. Stem Cells Applications in Regenerative Medicine and Disease Therapeutics. Int J Cell Biol. 2016;2016:6940283. doi:10.1155/2016/6940283
Mattei V, Martellucci S, Pulcini F, Santilli F, Sorice M, Delle Monache S. Regenerative Potential of DPSCs and Revascularization: Direct, Paracrine or Autocrine Effect?. Stem Cell Rev Rep. 2021;17(5):1635-1646. doi:10.1007/s12015-021-10162-6
Mita T, Furukawa-Hibi Y, Takeuchi H, et al. Conditioned medium from the stem cells of human dental pulp improves cognitive function in a mouse model of Alzheimer's disease. Behav Brain Res. 2015;293:189-197. doi:10.1016/j.bbr.2015.07.043
Nito C, Suda S, Nitahara-Kasahara Y, Okada T, Kimura K. Dental-Pulp Stem Cells as a Therapeutic Strategy for Ischemic Stroke. Biomedicines. 2022;10(4):737. Published 2022 Mar 22. doi:10.3390/biomedicines10040737
Romito A, Cobellis G. Pluripotent Stem Cells: Current Understanding and Future Directions. Stem Cells Int. 2016;2016:9451492. doi:10.1155/2016/9451492
Rothschild J. Ethical considerations of gene editing and genetic selection. J Gen Fam Med. 2020;21(3):37-47. Published 2020 May 29. doi:10.1002/jgf2.321
Shi J, Zhao YC, Niu ZF, et al. Mesenchymal stem cell-derived small extracellular vesicles in the treatment of human diseases: Progress and prospect. World J Stem Cells. 2021;13(1):49-63. doi:10.4252/wjsc.v13.i1.49
Staniowski T, Zawadzka-Knefel A, Skośkiewicz-Malinowska K. Therapeutic Potential of Dental Pulp Stem Cells According to Different Transplant Types. Molecules. 2021;26(24):7423. Published 2021 Dec 7. doi:10.3390/molecules26247423
Szeto JY, Lewis SJ. Current Treatment Options for Alzheimer's Disease and Parkinson's Disease Dementia. Curr Neuropharmacol. 2016;14(4):326-338. doi:10.2174/1570159x14666151208112754
Wang F, Jia Y, Liu J, et al. Dental pulp stem cells promote regeneration of damaged neuron cells on the cellular model of Alzheimer's disease. Cell Biol Int. 2017;41(6):639-650. doi:10.1002/cbin.10767
Wang J, Zuzzio K, Walker CL. Systemic Dental Pulp Stem Cell Secretome Therapy in a Mouse Model of Amyotrophic Lateral Sclerosis. Brain Sci. 2019;9(7):165. Published 2019 Jul 14. doi:10.3390/brainsci9070165
Yamada Y, Nakamura-Yamada S, Kusano K, Baba S. Clinical Potential and Current Progress of Dental Pulp Stem Cells for Various Systemic Diseases in Regenerative Medicine: A Concise Review. Int J Mol Sci. 2019;20(5):1132. Published 2019 Mar 6. doi:10.3390/ijms20051132
Yamamoto A, Sakai K, Matsubara K, Kano F, Ueda M. Multifaceted neuro-regenerative activities of human dental pulp stem cells for functional recovery after spinal cord injury. Neurosci Res. 2014;78:16-20. doi:10.1016/j.neures.2013.10.010