Clinical Profile and Outcome of Critically Ill Children in Tertiary Care Hospital
Main Article Content
Abstract
Introduction: The aim is to study the clinical profile and outcome of critically ill patients admitted to Pediatric Intensive Care Unit (PICU).
Method: This was a retrospective study of the demography, clinical profile and outcome of PICU patients admitted over a period of 1 year from January 2022 to December 2022.
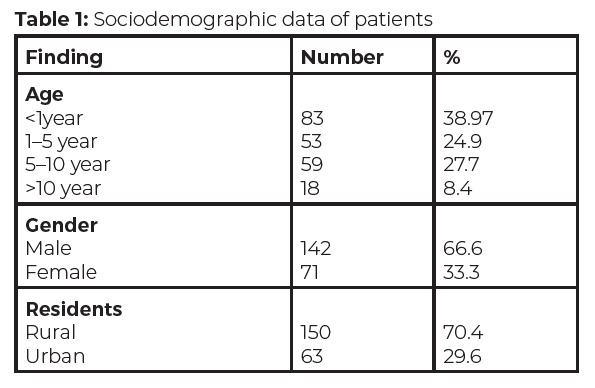
Result: Total 213 patients were admitted, with males and females 66.7% and 33.3%, respectively. 62% of the patients were below 5 years of age. The most common presentation was primary neurological abnormalities 22.1% followed by primary respiratory abnormality 20.2%. The majority of patients 79.9% improved and discharged, 3.8% expired, 13.2% were referred after stabilization, and 3.3% left against medical advice.
Conclusion: A most common cause of admission in PICU is primary neurological abnormalities followed by respiratory.
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Under Creative Commons the Authors retain ownership of the copyright for their content. The authors assign exclusive commercial re-use rights of the article to the Journal.
All open access articles published are distributed under the terms of the CC BY-NC 4.0 license (Creative Commons Attribution-Non-Commercial 4.0 International Public License as currently displayed at http://creativecommons.org/licenses/by-nc/4.0/legalcode) which permits unrestricted use, distribution, and reproduction in any medium, for non-commercial purposes, provided the original work is properly cited.
Authors agree to the open access publication policy of the Journal.
References
Lassi ZS, Mallick D, Das JK, et al. Essential interventions for child health. Reprod Health. 2014;11(1):4.
WHO. Pocket book for Hospital care for children: guidelines for the management of common illnesses
with limited resources. Geneva, Switzerland. World Health Organization; 2005.
Goldstein B, Giroir B, Randolph A, and the Members of the International Consensus Conference on Pediatric Sepsis. International pediatric sepsis consensus conference: definitions for sepsis and organ dysfunction in pediatrics. PediatrCrit Care Med 2005; 6: 2–8.
Young MP, Birkmeyer JD. Potential reduction in mortality rates using an intensivist model to manage intensive care units. Eff Clin Pract. 2000;3(6):284-9.
Fiser DH, Tilford JM, Roberson PK. Difference in pediatric ICU mortality risk over time. Crit Care Med. 1998;26:1737-43
Haque A, Bano S. Improving outcome in pediatric intensive care unit in academic hospital in Pakistan.
Pakistan J Med Sci. 2009;25:605-8.
Singhal D, Kumar N, Puliyl JM, Singh SK, Srinivas V. Prediction of mortality by application of PRISM score in intensive care unit. Indian Pediatr. 2001;38:714-9.
Shah GS, Shah BK, Thapa A, Shah L, Mishra OP. Admission patterns and outcome in a pediatric intensive care unit in Nepal. Br J Med Med Res. 2014;4(30):4939-45.
Haque A, Bano S. Clinical profile and outcome in a pediatric intensive care unit in Pakistan. J Coll Phys Surg Pakistan. 2009;19:534-5.
Blessing I, Iyoha A, Pooboni SK ,Vuppali NK. Morbidity pattern and outcome of patients admitted into a
pediatric intensive care unit in India. Ind J Clin Med. 2014;51-5.
Sahoo B, Patnaik S, Mishra R, Jain MK. Morbidity pattern and outcome of children admitted to a paediatric intensive care unit of Eastern India. Int J Contemp Pediatr 2017;4:486- 9.
Khilnani P, Sarma D, Singh. Demographic profile and outcome analysis of tertiary level pediatric intensive care unit. Indian J Paediatr. 2004;71:587- 91.
Bellad R, Rao S, Patil VD, Mahantshetti NS. Outcome of intensive care unit patients using pediatric risk of mortality (PRISM) score. Indian Pediatr. 2009;46:1091-2.
Choi KMS, Ng DKK, Wong SF. Assessment of the pediatric index of mortality (PIM) and the pediatric risk of mortality (PRISM) III score for prediction of mortality in a paediatric intensive care unit in Hong Kong. Hong Kong Med J. 2005;11:97-103.